Covid-19 Facts and Statistics for the General Public
As of April 6, 2021, this page is no longer being updated on a daily basis.
How does Covid-19 impact most Oklahomans? See our chart below for a rolling daily total of new positive tests and deaths. Scroll down for relevant facts about Covid-19 such as symptoms, who is most vulnerable, and mask effectiveness.
Treatment Alert: Politicians and the media appear reluctant to talk about monoclonal antibody treatments. The treatment is safe and effective, reducing the risk of hospitalization and death by 87% in COVID-19 patients, according to a recent study. To receive monoclonal antibody treatments, patients need a doctor’s prescription and must fall into the high-risk category- see “High-Risk Factors” below.
Search directory of infusion centers
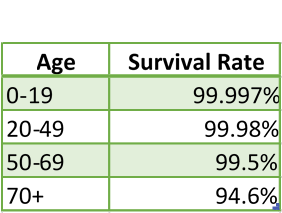
Best Estimate COVID Survival Rates by Age From the CDC
Oklahoma COVID-19 Daily New Positive Tests*/New Deaths
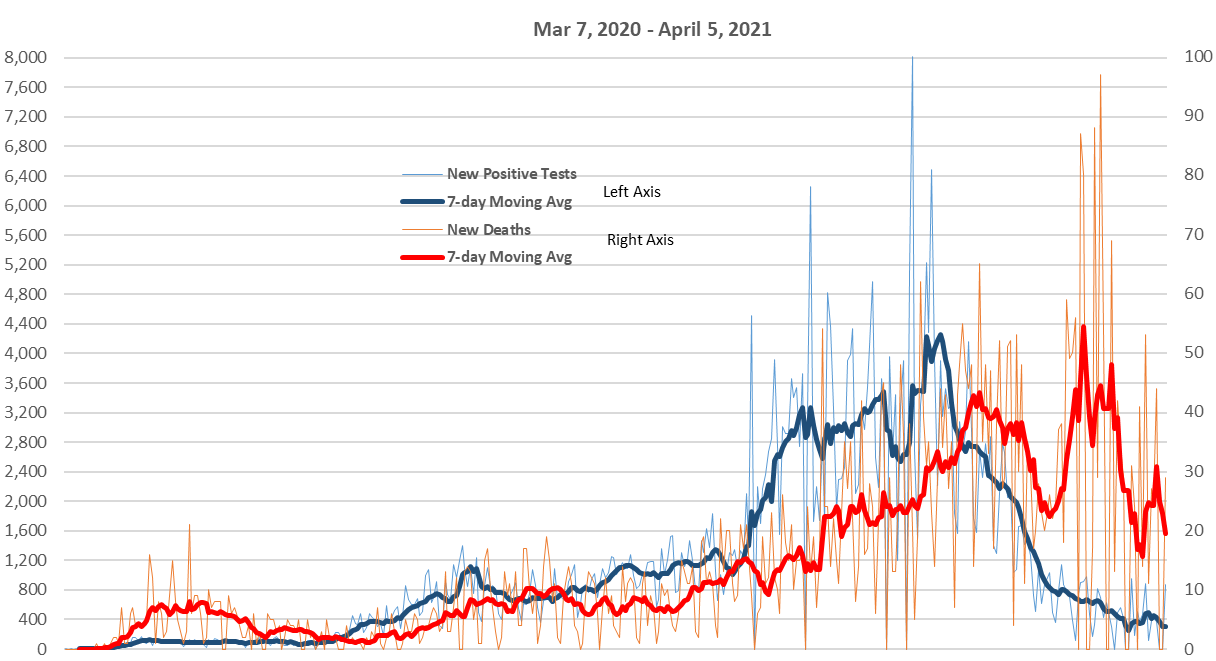
Note: The Covid Tracking Project ceased data collection on 3/7/21, starting on 3/8/21 data will be pulled from the Oklahoman’s COVID Tracker (https://www.oklahoman.com/
Note: Starting on 3/3/21 OKDOH started using the CDC’s Provisional Death Count to report COVID-19 deaths. As a part of this change they only update deaths via weekday emails. This may cause spikes in the data.
Unexpected Deaths
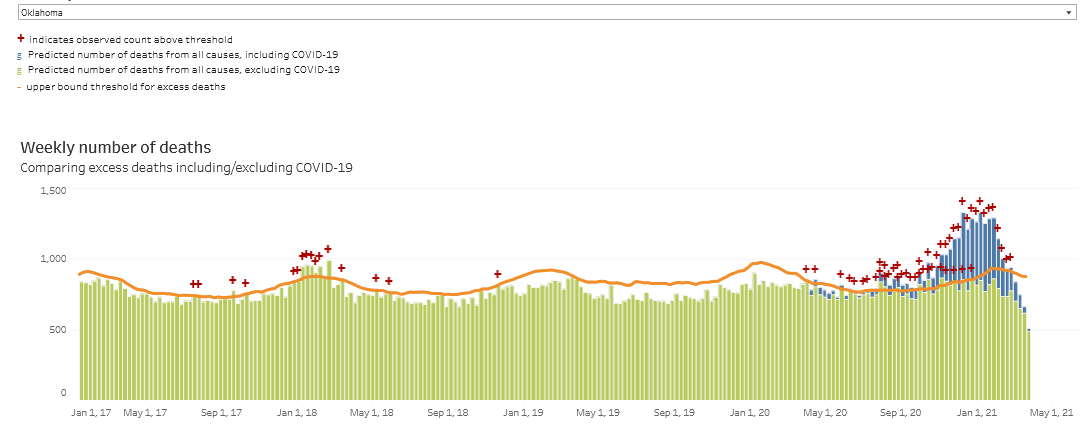
Unexpected deaths data from the CDC was updated 4/1/21.
The Centers for Disease Control produces a model of how many deaths each state might expect (weekly since January 2017), in the chart above from all causes given time of year and demographics. A “+” character indicates weeks with more deaths than expected compared to the upper end of a 95% confidence interval. https://www.cdc.gov/nchs/nvss/vsrr/covid19/excess_deaths.htm
Covid-19 Facts
Symptoms of Covid-19
- Fever/chills
- Cough
- Shortness of breath/difficulty breathing
- Fatigue
- Muscle/body aches
- Headache
- New loss of taste or smell
- Sore throat
- Congestion/runny nose
- Nausea/vomiting
- Diarrhea
Who is NOT vulnerable to Covid-19 (unlikely to suffer serious illness or death)?
- Older adults (in particular, those in frail health; see below)
- Individuals with underlying health problems – i.e. serious health conditions, which are commonly referred to as ‘comorbidities’ (see below)
High-Risk Factors
High risk is defined as patients who meet at least one of the following criteria:
- Have a body mass index (BMI) ≥35
- Have chronic kidney disease
- Have diabetes 2
- Have immunosuppressive disease
- Are currently receiving immunosuppressive treatment
- Are ≥65 years of age
- Are ≥55 years of age AND have
- cardiovascular disease, OR
- hypertension, OR
- chronic obstructive pulmonary disease/other chronic respiratory disease.
- Are 12 – 17 years of age AND have
- BMI ≥85th percentile for their age and gender based on CDC growth charts, https://www.cdc.gov/growthcharts/clinical_charts.htm, OR
- sickle cell disease, OR
- congenital or acquired heart disease, OR
- neurodevelopmental disorders, for example, cerebral palsy, OR
- a medical-related technological dependence, for example, tracheostomy, gastrostomy, or positive pressure ventilation (not related to COVID-19), OR
- asthma, reactive airway or other chronic respiratory disease that requires daily medication for control.
Age and Covid-19
- For children, the risk of dying from Covid-19 appears to be much less than that of dying from seasonal influenza and pneumonia
- U.K. and U.S. statistics show that the 0 to 19 age group’s share of Covid-19 deaths is very nearly zero.
- As experts have noted, a school age child is more likely to be hit by lightning than die of Covid-19
- Fatalities for people less than 65 years old without underlying health conditions are remarkably uncommon.
- The Covid-19 death rate for people less than 45 is very nearly zero percent.
- The median age of Americans who have died from Covid-19 is 80. Up to half of all deaths in the U.S. and Europe have occurred in nursing homes and elder care facilities.
- One analysis indicated 40 percent of Covid-19 deaths in the U.S. prior to June occurred in nursing homes.
- At least 2 states, New York and California, have required nursing homes to accept Covid-positive patients. New York has a higher Covid-19 death rate (per million population) than any nation or comparable region in the world.
- In terms of age, risk occurs for those over age 50, and becomes truly risky for those over age 70, very likely due to increased comorbidities that naturally occur with age. Risk rises with age, as do comorbidities. Death is extremely rare for teenagers.
Means of Transmission
- Mainly occurs from close person-to-person contact, with the virus expelled via airborne droplets during normal respiratory exhalation (i.e. breathing out) or via a cough or sneeze.
- In accordance with the World Health Organization’s pandemic mitigation guidelines, many countries are advising or requiring one meter (3 feet) of physical distance between individuals.
- In three feet, normal respiratory droplets (expelled by normal breathing) fall enough that it is unlikely for others to breathe in the droplets. Shouting, coughing, and sneezing cause droplets to travel farther. Face coverings shorten the travel distance. Smaller-than-normal droplets will travel farther.
- Small children are unlikely to pass the virus to adults.
- Touching a surface is also unlikely to result in Covid-19 infection.
- Asymptomatic transmission by infected individuals (i.e. individuals who test positive but do not have any symptoms) may occur but likely presents a low risk.
- Positive tests for the SARS-CoV-2 virus (Covid-19) may merely detect viral fragments in which a body’s immune system has already successfully eliminated a mild, largely asymptomatic, infection.
- About 80 percent of Covid-19 carriers infect no one. The danger lies in “super spread events” where one person infects many others in a group setting.
Masks (revised 8/4/20)
- The Netherlands’ “top scientists, having examined key data and research, have declared there is no firm evidence to back the use of face coverings.” (see article)
- The World Health Organization notes (see page 14 of this report) that there is NO scientifically-verified evidence that masks slow the spread of influenza virus (50 times larger than the virus that causes Covid-19), whether worn by asymptomatic or symptomatic individuals, but only recommends masks due to “mechanistic plausibility.”
- A May 2020 CDC publication notes: “Although mechanistic studies support the potential effect of hand hygiene or face masks, evidence from 14 randomized controlled trials of these measures did not support a substantial effect on transmission of laboratory-confirmed influenza.”
- CDC Director, Robert Redfield, appears to favor mask-wearing despite the evidence.
- It is presumed, but unconfirmed in real-world experiments, that masks worn by Covid-infected individuals can slow the spread of the virus by decreasing the distance respiratory droplets can travel. For those showing symptoms, best advice is to wear a mask and get tested.
- The uninfected might benefit from wearing masks in the presence of infected individuals. For those who are particularly vulnerable to Covid-19 (i.e. have comorbidities), best advice is to wear a mask when unable to socially distance. Properly fitted N95 masks are considered the best protection. These were in short supply, but are now readily available.
- Given the WHO and CDC conclusions (above) of no scientific evidence for mask efficacy, masks could provide a false sense of security, leading to unhealthy risk-taking. Thus, universal government-imposed mask mandates are questionable at best and could actually be harmful.
Lockdowns
- Historically, only the infected have been quarantined. The World Health Organization (WHO), in their October 2019 report about responding to an influenza-like pandemic, stated that quarantine was not recommended under any circumstances, due to the very low overall quality of evidence and the ethical concerns of restricting the free movement of healthy individuals.
- Quarantine involves forcefully isolating infected individuals or those who have had direct contact with infected individuals. WHO rightfully acknowledged the ethical concerns associated with mandatory quarantines of potentially exposed individuals; they did not even contemplate taking such extreme measures against healthy individuals with no known or presumed exposure to the virus.
- Economic/social lockdowns, including closing schools and churches, are something akin to house arrest of healthy people.
- Lockdowns have resulted in more social isolation, resulting in more suicides, greater alcohol use, and more incidents of domestic violence.
- A U.N. study points out that shutdowns over Covid-19, producing economic recession and reversing 2 to 3 years of economic gains, will kill hundreds of thousands of children (otherwise largely untouched by the virus) and put millions back into extreme poverty.
Herd Immunity
- Herd immunity occurs once a large enough fraction of population has developed adequate antibodies (i.e. ‘immunity’, which can be temporary, lasting a few months or a few years or many years) such that, on average, an infected person infects fewer than one additional individual. This is because so many others are already immune.
- This provides a measure of protection for those who are not immune because the likelihood of meeting someone with an active, contagious infection is low.
- If individuals at very low risk (healthy, below the age of 65) had been allowed to become infected in high enough numbers, while the vulnerable sheltered in place, herd immunity could likely have been achieved by now.
- NOTE: Respiratory viral pandemics end with herd immunity. Stopping the spread altogether through means other than a vaccine is therefore an unrealistic goal.
Facts researched and assembled by 1889 Institute staff with the aid of Steve Trost, Associate Director of the Institute for the Study of Free Enterprise, Oklahoma State University and William Paiva, Executive Director of Center For Health Systems Innovation, Patterson Foundation Chair, Spears School of Business and Center for Health Sciences, Oklahoma State University.
Policy Conclusions Given the Facts (revised 8/4/20)
- Do NOT Lock Down.
- Keep Schools Open.
- The American Academy of Pediatric guidelines point out that the social and emotional costs to children of not being in school far outweigh the health risk to children or adults who are around them.
- If need-be, furlough vulnerable public education employees, perhaps with partial pay, for one month after school restarts.
- This helps to develop herd immunity so that the vulnerable and their caregivers can eventually move about in relative safety.
- Publicize what makes one vulnerable (comorbidities/age) and encourage them to shelter.
- Take steps to protect those in nursing homes through frequent testing and worker screening as well as N95 mask wearing.
- Encourage social distancing but reduce the distance consistent with WHO guidelines.
- Encourage frequent hand washing.
- Publicize facts about risks and let individuals decide on mask wearing (including individual businesses’ policies) EXCEPT, perhaps, where social distancing is not possible, such as on public transportation.
- ANYONE showing ANY symptoms at all, including lost sense of smell, unexplained fatigue, diarrhea, or anything like a cold should STAY HOME. If being out is necessary, WEAR a mask and STAY AWAY from large groups in small areas. Older people should be especially avoided.
- Caregivers for the vulnerable should shelter as much as possible and take special precautions. Only N95 masks are likely to provide protection.
